- Record: found
- Abstract: found
- Article: found
Autoimmunity is a hallmark of post-COVID syndrome

Read this article at
Abstract
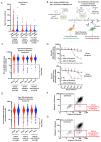
Autoimmunity has emerged as a characteristic of the post-COVID syndrome (PCS), which may be related to sex. In order to further investigate the relationship between SARS-CoV-2 and autoimmunity in PCS, a clinical and serological assessment on 100 patients was done. Serum antibody profiles against self-antigens and infectious agents were evaluated by an antigen array chip for 116 IgG and 104 IgM antibodies. Thirty pre-pandemic healthy individuals were included as a control group. The median age of patients was 49 years (IQR: 37.8 to 55.3). There were 47 males. The median post-COVID time was 219 (IQR: 143 to 258) days. Latent autoimmunity and polyautoimmunity were found in 83% and 62% of patients, respectively. Three patients developed an overt autoimmune disease. IgG antibodies against IL-2, CD8B, and thyroglobulin were found in more than 10% of the patients. Other IgG autoantibodies, such as anti-interferons, were positive in 5–10% of patients. Anti-SARS-CoV-2 IgG antibodies were found in > 85% of patients and were positively correlated with autoantibodies, age, and body mass index (BMI). Few autoantibodies were influenced by age and BMI. There was no effect of gender on the over- or under-expression of autoantibodies. IgG anti-IFN-λ antibodies were associated with the persistence of respiratory symptoms. In summary, autoimmunity is characteristic of PCS, and latent autoimmunity correlates with humoral response to SARS-CoV-2.
Related collections
Most cited references11
- Record: found
- Abstract: found
- Article: found
Autoantibodies neutralizing type I IFNs are present in ~ 4% of uninfected individuals over 70 years and account for ~ 20% of COVID-19 deaths

- Record: found
- Abstract: found
- Article: found
New-onset IgG autoantibodies in hospitalized patients with COVID-19
- Record: found
- Abstract: found
- Article: not found