- Record: found
- Abstract: found
- Article: found
The Effect of Changing Patterns of Obstetric Care in Scotland (1980–2004) on Rates of Preterm Birth and Its Neonatal Consequences: Perinatal Database Study

Read this article at
Abstract
Jane Norman and colleagues analyzed linked perinatal surveillance data in Scotland and find that between 1980 and 2004 increases in spontaneous and medically induced preterm births contributed equally to the rising rate of preterm births.
Abstract
Background
Rates of preterm birth are rising worldwide. Studies from the United States and Latin America suggest that much of this rise relates to increased rates of medically indicated preterm birth. In contrast, European and Australian data suggest that increases in spontaneous preterm labour also play a role. We aimed, in a population-based database of 5 million people, to determine the temporal trends and obstetric antecedents of singleton preterm birth and its associated neonatal mortality and morbidity for the period 1980–2004.
Methods and Findings
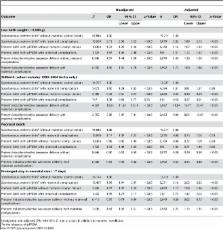
There were 1.49 million births in Scotland over the study period, of which 5.8% were preterm. We found a percentage increase in crude rates of both spontaneous preterm birth per 1,000 singleton births (10.7%, p<0.01) and medically indicated preterm births (41.2%, p<0.01), which persisted when adjusted for maternal age at delivery. The greater proportion of spontaneous preterm births meant that the absolute increase in rates of preterm birth in each category were similar. Of specific maternal complications, essential and pregnancy-induced hypertension, pre-eclampsia, and placenta praevia played a decreasing role in preterm birth over the study period, with gestational and pre-existing diabetes playing an increasing role. There was a decline in stillbirth, neonatal, and extended perinatal mortality associated with preterm birth at all gestation over the study period but an increase in the rate of prolonged hospital stay for the neonate. Neonatal mortality improved in all subgroups, regardless of obstetric antecedent of preterm birth or gestational age. In the 28 wk and greater gestational groups we found a reduction in stillbirths and extended perinatal mortality for medically induced but not spontaneous preterm births (in the absence of maternal complications) although at the expense of a longer stay in neonatal intensive care. This improvement in stillbirth and neonatal mortality supports the decision making behind the 34% increase in elective/induced preterm birth in these women. Although improvements in neonatal outcomes overall are welcome, preterm birth still accounts for over 66% of singleton stillbirths, 65% of singleton neonatal deaths, and 67% of infants whose stay in the neonatal unit is “prolonged,” suggesting this condition remains a significant contributor to perinatal mortality and morbidity.
Conclusions
In our population, increases in spontaneous and medically induced preterm births have made equal contributions to the rising rate of preterm birth. Despite improvements in related perinatal mortality, preterm birth remains a major obstetric and neonatal problem, and its frequency is increasing.
Editors' Summary
Background
Most pregnancies last about 40 weeks but increasing numbers of babies are being born preterm, before they reach 37 weeks of gestation (gestation is the period during which a baby develops in its mother). Nowadays in the US, for example, more than half a million babies arrive earlier than expected every year (1 in 8 babies). Although improvements in the care of newborn babies (neonatal care) mean that preterm babies are more likely to survive than in the past, preterm birth remains the single biggest cause of infant death in many developed countries, and many preterm babies who survive have long-term health problems and disabilities, particularly those born before 32 weeks of gestation. Preterm births can be spontaneous or medically induced. At present, it impossible to predict which mothers will spontaneously deliver early and there is no effective way to prevent these preterm births; medically induced early labor is undertaken when either the unborn baby or mother would be at risk if the pregnancy continued to full term.
Why Was This Study Done?
Preterm birth rates need to be reduced, but before this can be done it is important to know how the causes of preterm birth, the numbers of preterm stillbirths, and the numbers of preterm babies who die at birth (neonatal deaths) or soon after (perinatal deaths) are changing with time. If, for example, the rise in preterm births is mainly due to an increase in medically induced labor and if this change in practice has reduced neonatal deaths, it would be unwise to try to reduce the preterm birth rate by discouraging medically induced preterm births. So far, data from the US and Latin America suggest that the increase in preterm births in these countries is solely due to increased rates of medically induced preterm births. However, in Europe and Australia, the rate of spontaneous preterm births also seems to be increasing. In this study, the researchers examine the trends over time and causes of preterm birth and of neonatal death and illness in Scotland over a 25-year period.
What Did the Researchers Do and Find?
By searching a Scottish database of linked maternity records and infant health and death records, the researchers identified 1.49 million singleton births that occurred between 1980 and 2004 of which nearly 90,000 were preterm births. Over the study period, the rates of spontaneous and of medically induced preterm births per 1,000 births increased by 10.7% and 41.2%, respectively, but because there were more spontaneous preterm births than medically induced preterm births, the absolute increase in the rates of each type of birth was similar. Several maternal complications including preeclampsia (a condition that causes high blood pressure) and placenta previa (covering of the opening of the cervix by the placenta) played a decreasing role in preterm births over the study period, whereas gestational and preexisting diabetes played an increasing role. Finally, there was a decline in stillbirths and in neonatal and perinatal deaths among preterm babies, although more babies remained in the hospital longer than 7 days after birth. More specifically, after 28 weeks of gestation, stillbirths and perinatal deaths decreased among medically induced preterm births but not among spontaneous preterm births.
What Do These Findings Mean?
These findings indicate that in Scotland between 1980 and 2004, increases in spontaneous and medically induced preterm births contributed equally to the rising rate of preterm births. Importantly, they also show that the increase in induced preterm births helped to reduce stillbirths and neonatal and perinatal deaths, a finding that supports the criteria that clinicians currently use to decide whether to induce an early birth. Nevertheless, preterm births still account for two-thirds of all stillbirths, neonatal deaths, and extended neonatal stays in hospital and thus cause considerable suffering and greatly increase the workload in neonatal units. The rates of such births consequently need to be reduced and, for Scotland at least, ways will have to be found to reduce the rates of both spontaneous and induced preterm births to achieve this goal while continuing to identify those sick babies who need to be delivered early to give them the best chance of survival.
Additional Information
Please access these Web sites via the online version of this summary at http://dx.doi.org/10.1371/journal.pmed.1000153
-
Tommys is a nonprofit organization that funds research and provides information on the causes and prevention of miscarriage, premature birth, and stillbirth
-
The March of Dimes, a nonprofit organization for pregnancy and baby health, provides information on preterm birth (in English and Spanish)
-
The Nemours Foundation, another nonprofit organization for child health, also provides information on premature babies (in English and Spanish)
-
The US Centers for Disease Control and Prevention provides information on maternal and infant health (in English and Spanish)
-
The US National Women's Health Information Center has detailed information about pregnancy, including a section on pregnancy complications
-
MedlinePlus provides links to other information on premature babies and to information on pregnancy (in English and Spanish)
Related collections
Most cited references9
- Record: found
- Abstract: found
- Article: not found
Trends in preterm birth and perinatal mortality among singletons: United States, 1989 through 2000.
- Record: found
- Abstract: found
- Article: not found
Caesarean section and risk of unexplained stillbirth in subsequent pregnancy.
- Record: found
- Abstract: found
- Article: found