- Record: found
- Abstract: found
- Article: found
Global Burden of Congenital Heart Disease: Experience in Korea as a Potential Solution to the Problem
editorial
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
Congenital heart disease (CHD) is the most common congenital anomaly, accounting for
almost 30% of all major birth defects. Reported birth prevalence of CHD worldwide
is around 9 per 1,000 live births, with significant geographical differences.1) The
highest CHD birth prevalence was reported in Asia, with 9.3 per 1,000 live births,
whereas 8.2 and 6.9 per 1,000 live births in Europe and North America, respectively.1)
The incidence of ‘significant CHD’, which will require surgery before one year of
age, was reported to be 3.2/1,000 live births in a population based study in North
America.2) A worldwide annual birth rate is around 150 million, which corresponds
to 1.35 million live births with CHD and 480,000 births with significant CHDs every
year.2)
3)
In 2017, 5.4 million children under 5 years of age died worldwide, of whom 214,214
children with CHD died, representing 3.97% of all causes of death and 31.5 deaths
per 100,000 poplulation.4) The overall mortality rates in children has declined significantly,
by half globally over the past two decades, but deaths and disabilities in children
with CHD have been steadily increased in countries with low incomes and high fertility
rates.4)
5) There are the wide disparities of health system resources to treat CHD between
countries, in terms of per capita income, education level, fertility rate, and pediatric
cardiac experts and cardiovascular centers.4)
6) Indeed, about 90% of CHD patients do not have adequate access to diagnosis and
treatment, and 75% do not have access to cardiac surgery worldwide, indicating that
CHD is still a great health care burden worldwide.6)
7)
8)
In this issue of the Korean Circulation Journal, Shin et al.9) reported the recent
surgical outcomes of CHD in Korea based on the Korea Heart Foundation (KHF) data.
The surgical data of 6,599 CHD patients with financial support from KHF in the recent
15-year period (2000–2014, the recent era) were analyzed and compared with those of
the previous reports on patients who had CHD surgery from 1984 to 1999 (the past era).
This study population represents about 12% of all CHD surgical volume in Korea during
the same period, in which 54,144 CHD surgeries were performed, based on the KHF Annual
Report on “The Present Status of Cardiovascular Surgery in Korea”.10) Given that no
national data on surgical outcomes is available until recently, we may assume that
the results of this study represents trends in CHD surgical outcomes over the last
three decades in Korea.
The main finding of the study is surgical mortality rates by age at surgery and diagnosis.
Compared to mortality rates in the past era, the overall mortality rates decreased
significantly in the recent era, with an early mortality rate of 3.8% (vs. 8.6% in
the past era) and late mortality rate of 1.8% (vs. 5.3%). Especially, substantial
improvements were achieved in patients under one year of age at surgery. Compared
with mortality rates in the past era, early mortality rates in neonates, patients
under 3 months of age, and infants have decreased significantly, with 12.2% (vs. 29.7%
in the past era), 8.2% (vs. 23.0%), and 6.0% (vs. 15.8%), respectively. Mortality
rates in patients over 1 year of age ranged from 1.8% to 3.0%.
It is also noteworthy that the volume of neonatal surgical cases has increased significantly
in the recent era with 491 patients (7.4% of all patients), while 74 patients (0.6%)
in the past era. About 30% of neonatal surgeries were palliative procedures for complex
CHD. The most common diagnosis in neonatal surgery was coarctation of the aorta or
interrupted aortic arch (15.9%), followed by transposition of the great arteries (14.7%)
and pulmonary atresia with ventricular septal defect (10.8%). It is encouraging that
surgical outcomes improved substantially in neonates with more complex CHD, which
needed more complicated surgical procedures in the recent era. Nevertheless, mortality
rates were still relatively high (>10%) in patients with hypoplastic left heart syndrome,
total anomalous pulmonary venous return, congenitally-corrected transposition of the
great arteries, and some aortic diseases (diagnosis not specified).
Lastly, another notable data is the number of overseas patients, with 491 patients
(7.4% of all patients) from 30 countries, mainly nearby Asian countries. As the health
care system and resources improved dramatically during the past two decades, recent
overall surgical outcomes have improved significantly in Korea, while there is still
a great shortage of resources to treat these patients in some countries worldwide.
Treatment of CHD by surgery or intervention is always relatively expensive, requiring
specialized equipment and facilities, and well-trained pediatric cardiologists and
cardiac surgeons. Most patients with CHD require life-long follow up and care, furthermore
many patients also need additional surgeries or interventions. Given that the incidence
of CHD is similar worldwide, the burden of treating these patients is very challenging
in countries with low oncome and high fertility rates.6) In addition, in underdeveloped
countries infectious diseases and nutritional deficiencies are the major causes of
death, while CHD accounts for a small portion of childhood mortality, less than 5%
of all-cause mortality, which result in insufficient investment in CHD treatment.4)
6) Until the early 1980s, the burden of CHD in Korea was quite high. In 1984, the
year KHF was established, the gross national income per capita was $2,378 and the
annual birth rate was 675,000 (Korean Statistical Information Service, http://kosis.kr/search/search.do).
Some of the CHD patients had to go abroad to undergo surgery at the time, mainly due
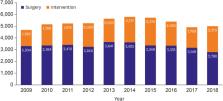
to financial difficulties. Since the establishment of KHF, the volume of CHD surgery
or intervention has increased dramatically, and in 2014, a total of 5,802 surgeries
or interventions were performed with a total mortality rate of only 1.6% (Figure 1).10)
The great achievements in the treatment of CHD in Korea are thought to be fueled by
the support of KHF, and have been boosted by increase in per capita income, the national
health insurance system, decrease in fertility rate, and high education level. These
experiences in Korea could be potential solutions to decrease the burdens of CHD treatment
in underdeveloped countries. However, this is a very complex problem because those
countries have more urgent socio-economic and other public health issues than CHD.4)
6) Given that the main barriers to the treatment of CHD are poverty and limited manpower,
especially cardiac surgeons, it will be difficult and time consuming to improve the
situations. Therefore, as Korea has been doing recently, a practical, but not fundamental,
way for solving the problems at this time is that developed countries invite CHD patients
for surgery, invite medical staffs for training, or have medical teams go to underdeveloped
countries, treat patients, and help train local doctors.
Currently, CHD is not a ‘burden’ in Korea. As the authors concluded, surgical outcomes
improved significantly, comparable to those of other developed countries, and Korea
has become a country to help other underdeveloped countries. Obviously, this achievement
was made through the great socio-economic development of Korea. Additionally, I believe
that the dedication of Korean doctors to care for CHD patients also contributed to
that. Because the burden of CHD in underdeveloped countries are still serious, international
cooperation is urgently needed to increase investments in pediatric cardiac care across
the world.5)
Related collections
Most cited references5
- Record: found
- Abstract: found
- Article: not found
The incidence of congenital heart disease.
Julien Hoffman, Samuel Kaplan (2002)
- Record: found
- Abstract: found
- Article: not found
The improvement of care for paediatric and congenital cardiac disease across the World: a challenge for the World Society for Pediatric and Congenital Heart Surgery.
- Record: found
- Abstract: not found
- Article: not found
The invisible child: childhood heart disease in global health
Bistra Zheleva, J Atwood (2017)