- Record: found
- Abstract: found
- Article: found
Prevalence of Hashimoto Thyroiditis in Adults With Papillary Thyroid Cancer and Its Association With Cancer Recurrence and Outcomes
Read this article at
Abstract
his cohort study assesses the prevalence of and outcomes associated with Hashimoto thyroiditis among adults with papillary thyroid cancer.
Key Points
Question
Is Hashimoto thyroiditis associated with papillary thyroid cancer characteristics and outcomes?
Findings
In this cohort study of 9210 patients with papillary thyroid cancer, 19% had Hashimoto thyroiditis. Patients with Hashimoto thyroiditis had less aggressive papillary thyroid cancer tumors, lower rates of tumor recurrence, and lower disease-related mortality compared with patients without Hashimoto thyroiditis.
Abstract
Importance
Hashimoto thyroiditis (HT) has been suggested to be associated with papillary thyroid cancer (PTC) development. However, its association with PTC progression remains unclear.
Design, Setting, and Participants
This retrospective cohort study included a review of patients aged 18 to 75 years who had pathologically confirmed PTC treated at a single center in China from January 1, 2001, to December 31, 2014. Data analysis was performed from November 1 to December 31, 2020.
Main Outcomes and Measures
The primary outcome was the association of HT with PTC-related mortality, assessed using Cox proportional hazards regression models. The secondary outcome was the association of HT with aggressive characteristics and structural recurrence of PTC, assessed using logistic regression and Cox proportional hazards regression with and without adjustment for related factors.
Results
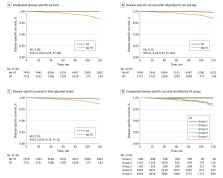
Of 9210 patients with PTC (mean [SD] age, 43.6 [12.0] years; 6872 [75%] women) included in the analysis, 1751 (19%) had HT. In the logistic regression model, HT was negatively associated with frequencies of primary tumor size of 4 cm or greater (adjusted odds ratio [aOR], 0.20; 95% CI, 0.12-0.33; P < .001), gross extrathyroidal extension (aOR, 0.44; 95% CI, 0.36-0.54; P < .001), extranodal extension (aOR, 0.66; 95% CI, 0.55-0.80; P < .001), and distant metastasis (aOR, 0.17; 95% CI, 0.04-0.71; P = .02). After a median follow-up of 85 months (range, 12-144 months), 131 PTC-related deaths were identified in the cohort; 2 patients who died had HT. Patients with HT had significantly superior outcomes compared with patients without HT in terms of unadjusted 10-year disease-specific survival (99.9% vs 96.6%; log-rank P < .001) and recurrence-free survival (92.0% vs 87.6%; log-rank P = .001). After adjusting for sex, age, primary tumor size, extrathyroidal extension, lymph node metastasis, distant metastasis, extent of surgery, and radioactive iodine ablation, HT was associated with decreased PTC-related mortality (hazard ratio [HR], 0.19; 95% CI, 0.05-0.76; P = .02). Stratified analysis showed that HT was associated with less frequent structural recurrence in patients with extrathyroidal extension (HR, 0.52; 95% CI, 0.38-0.71; P < .001; P = .002 for interaction) or after total thyroidectomy (HR, 0.50; 95% CI, 0.35-0.69; P < .001; P = .009 for interaction).
Related collections
Most cited references27
- Record: found
- Abstract: found
- Article: not found
Cancer statistics in China, 2015.
- Record: found
- Abstract: found
- Article: not found
2015 American Thyroid Association Management Guidelines for Adult Patients with Thyroid Nodules and Differentiated Thyroid Cancer: The American Thyroid Association Guidelines Task Force on Thyroid Nodules and Differentiated Thyroid Cancer.
- Record: found
- Abstract: found
- Article: not found