- Record: found
- Abstract: found
- Article: not found
Is HIV Infection a Risk Factor for Multi-Drug Resistant Tuberculosis? A Systematic Review
Read this article at
Abstract
Background
Tuberculosis (TB) is an important cause of human suffering and death. Human immunodeficiency virus (HIV), multi-drug resistant TB (MDR-TB), and extensive drug resistant tuberculosis (XDR-TB) have emerged as threats to TB control. The association between MDR-TB and HIV infection has not yet been fully investigated. We conducted a systematic review and meta-analysis to summarize the evidence on the association between HIV infection and MDR-TB.
Methods and Results
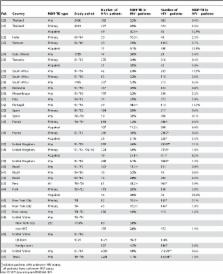
Original studies providing Mycobacterium tuberculosis resistance data stratified by HIV status were identified using MEDLINE and ISI Web of Science. Crude MDR-TB prevalence ratios were calculated and analyzed by type of TB (primary or acquired), region and study period. Heterogeneity across studies was assessed, and pooled prevalence ratios were generated if appropriate. No clear association was found between MDR-TB and HIV infection across time and geographic locations. MDR-TB prevalence ratios in the 32 eligible studies, comparing MDR-TB prevalence by HIV status, ranged from 0.21 to 41.45. Assessment by geographical region or study period did not reveal noticeable patterns. The summary prevalence ratios for acquired and primary MDR-TB were 1.17 (95% CI 0.86, 1.6) and 2.72 (95% CI 2.03, 3.66), respectively. Studies eligible for review were few considering the size of the epidemics. Most studies were not adjusted for confounders and the heterogeneity across studies precluded the calculation of a meaningful overall summary measure.
Conclusions
We could not demonstrate an overall association between MDR-TB and HIV or acquired MDR-TB and HIV, but our results suggest that HIV infection is associated with primary MDR-TB. Future well-designed studies and surveillance in all regions of the world are needed to better clarify the relationship between HIV infection and MDR-TB.
Related collections
Most cited references56
- Record: found
- Abstract: found
- Article: not found
Risk factors for multidrug resistant tuberculosis in Europe: a systematic review.
- Record: found
- Abstract: found
- Article: not found
HIV infection and multidrug-resistant tuberculosis: the perfect storm.
- Record: found
- Abstract: found
- Article: not found
