- Record: found
- Abstract: found
- Article: not found
Integrated and patient-centred management of Parkinson's disease: a network model for reshaping chronic neurological care
Read this article at
Abstract
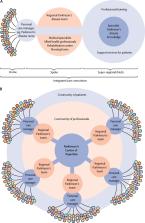
Chronic neurological diseases are the leading cause of disability globally. Yet, our health-care systems are not designed to meet the needs of many patients with chronic neurological conditions. Care is fragmented with poor interdisciplinary collaboration and lack of timely access to services and therapies. Furthermore, care is typically reactive, and complex problems are managed inadequately because of a scarcity of disease-specific expertise and insufficient use of non-pharmacological interventions. Treatment plans tend to focus on the disease rather than the individual living with it, and patients are often not involved in clinical decision making. By use of Parkinson's disease as a model condition, we show an integrated care concept with a patient-centred perspective that includes evidence-based solutions to improve health-care delivery for people with chronic neurological conditions. We anticipate that this integrated care model will improve the quality of life for patients, create a positive working environment for health-care professionals, and be affordable.
Related collections
Most cited references97

- Record: found
- Abstract: found
- Article: found
Global, regional, and national burden of neurological disorders, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016

- Record: found
- Abstract: found
- Article: found
Global, regional, and national burden of Parkinson's disease, 1990–2016: a systematic analysis for the Global Burden of Disease Study 2016
- Record: found
- Abstract: found
- Article: not found
