- Record: found
- Abstract: found
- Article: found
Acute maternal stress in pregnancy and schizophrenia in offspring: A cohort prospective study
Read this article at
Abstract
Schizophrenia has been linked with intrauterine exposure to maternal stress due to bereavement, famine and major disasters. Recent evidence suggests that human vulnerability may be greatest in the first trimester of gestation and rodent experiments suggest sex specificity. We aimed to describe the consequence of an acute maternal stress, through a follow-up of offspring whose mothers were pregnant during the Arab-Israeli war of 1967. A priori, we focused on gestational month and offspring's sex.
In a pilot study linking birth records to Israel's Psychiatric Registry, we analyzed data from a cohort of 88,829 born in Jerusalem in 1964–76. Proportional hazards models were used to estimate the relative risk (RR) of schizophrenia, according to month of birth, gender and other variables, while controlling for father's age and other potential confounders. Other causes of hospitalized psychiatric morbidity (grouped together) were analyzed for comparison.
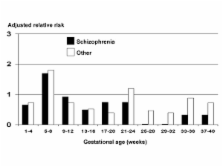
There was a raised incidence of schizophrenia for those who were in the second month of fetal life in June 1967 (RR = 2.3, 1.1–4.7), seen more in females (4.3, 1.7–10.7) than in males (1.2, 0.4–3.8). Results were not explained by secular or seasonal variations, altered birth weight or gestational age. For other conditions, RRs were increased in offspring who had been in the third month of fetal life in June 1967 (2.5, 1.2–5.2), also seen more in females (3.6, 1.3–9.7) than males (1.8, 0.6–5.2).
These findings add to a growing literature, in experimental animals and humans, attributing long term consequences for offspring of maternal gestational stress. They suggest both a sex-specificity and a relatively short gestational time-window for gestational effects on vulnerability to schizophrenia.
Related collections
Most cited references42
- Record: found
- Abstract: found
- Article: not found
Rates of adult schizophrenia following prenatal exposure to the Chinese famine of 1959-1961.
- Record: found
- Abstract: found
- Article: not found
Mechanisms of disease: glucocorticoids, their placental metabolism and fetal 'programming' of adult pathophysiology.
- Record: found
- Abstract: found
- Article: not found