- Record: found
- Abstract: found
- Article: found
Associations between multimorbidity and glycaemia (HbA1c) in people with type 2 diabetes: cross-sectional study in Australian general practice
Read this article at
Abstract
Objectives
To explore the prevalence of multimorbidity as well as individual and combinations of long-term conditions (LTCs) in people with type 2 diabetes (T2D) attending Australian general practice, using electronic health record (EHR) data. We also examine the association between multimorbidity condition count (total/concordant(T2D related)/discordant(unrelated)) and glycaemia (glycated haemoglobin, HbA1c).
Participants
69 718 people with T2D with a general practice encounter between 2013 and 2015 captured in the MedicineInsight database (EHR Data from 557 general practices and >3.8 million Australian patients).
Primary and secondary outcome measures
Prevalence of multimorbidity, individual and combinations of LTCs. Multivariable linear regression models used to examine associations between multimorbidity counts and HbA1c (%).
Results
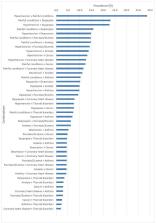
Mean (SD) age 66.42 (12.70) years, 46.1% female and mean (SD) HbA1c 7.1 (1.4)%. More than 90% of participants with T2D were living with multimorbidity. Discordant conditions were more prevalent (83.4%) than concordant conditions (69.9 %). The three most prevalent discordant conditions were: painful conditions (55.4%), dyspepsia (31.6%) and depression (22.8%). The three most prevalent concordant conditions were hypertension (61.4%), coronary heart disease (17.1%) and chronic kidney disease (8.5%). The three most common combinations of conditions were: painful conditions and hypertension (38.8%), painful conditions and dyspepsia (23.1%) and hypertension and dyspepsia (22.7%). We found no associations between any multimorbidity counts (total, concordant and discordant) or combinations and HbA1c.
Conclusions
Multimorbidity was common in our cohort of people with T2D attending Australian general practice, but was not associated with glycaemia. Although we did not explore mortality in this study, our results suggest that the increased mortality in those with multimorbidity and T2D observed in other studies may not be linked to glycaemia. Interestingly, discordant conditions were more prevalent than concordant conditions with painful conditions being the second most common comorbidity. Better understanding of the implications of different patterns of multimorbidity in people with T2D will allow more effective tailored care.
Related collections
Most cited references32
- Record: found
- Abstract: found
- Article: not found
Epidemiology of multimorbidity and implications for health care, research, and medical education: a cross-sectional study.
- Record: found
- Abstract: found
- Article: not found
10-year follow-up of intensive glucose control in type 2 diabetes.
- Record: found
- Abstract: found
- Article: not found