- Record: found
- Abstract: found
- Article: found
Predicting metachronous liver metastasis in patients with colorectal cancer: development and assessment of a new nomogram
Read this article at
Abstract
Background
We aimed to develop and validate a nomogram model, which could predict metachronous liver metastasis in colorectal cancer within two years after diagnosis.
Methods
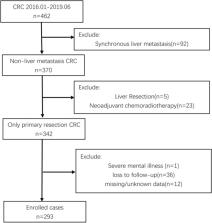
A retrospective study was performed on colorectal cancer patients who were admitted to Beijing Shijitan Hospital from January 1, 2016 to June 30, 2019. The least absolute shrinkage and selection operator (LASSO) regression model was used to optimize feature selection for susceptibility to metachronous liver metastasis in colorectal cancer. Multivariable logistic regression analysis was applied to establish a predictive model through incorporating features selected in the LASSO regression model. C-index, receiver operating characteristic (ROC) curve, calibration plot, and decision curve analysis (DCA) were employed to assess discrimination, distinctiveness, consistency with actual occurrence risk, and clinical utility of candidate predictive model. Internal validation was assessed with bootstrapping method.
Results
Predictors contained in candidate prediction nomogram included age, CEA, vascular invasion, T stage, N stage, family history of cancer, and KRAS mutation. This model displayed good discrimination with a C-index of 0.787 (95% confidence interval: 0.728–0.846) and good calibration, whereas area under the ROC curve (AUC) of 0.786. Internal validation obtained C-index of 0.786, and AUC of validation cohort is 0.784. Based on DCA, with threshold probability range from 1 to 60%; this predictive model might identify colorectal cancer metachronous liver metastasis to achieve a net clinical benefit.
Related collections
Most cited references55
- Record: found
- Abstract: not found
- Article: not found
Regularization Paths for Generalized Linear Models via Coordinate Descent
- Record: found
- Abstract: found
- Article: not found
Colorectal cancer statistics, 2020
- Record: found
- Abstract: found
- Article: not found