- Record: found
- Abstract: found
- Article: found
Fertility achieved through in vitro fertilization in a male patient with 48,XXYY syndrome
letter
De-Feng Liu
1 ,
Lian-Ming Zhao
2 ,
Kai Hong
2 ,
Jia-Ming Mao
1 ,
Yu-Zhuo Yang
1 ,
Zhe Zhang
2 ,
Hui Jiang
2
03 October 2017
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
Dear Editor,
The 48,XXYY syndrome is a rare sex chromosome aneuploidy with an incidence of 1:18
000–1:40 000 male births1 and is associated with hypergonadotropic hypogonadism as
an endocrine disorder.2
3 Most men with this syndrome are never diagnosed in China. Due to sex chromosome
aneuploidies and limited effective communication, these patients suffer from infertility.4
With a rare incidence rate, 48,XXYY syndrome is characterized by tall stature, abdominal
adiposity, and small testicles; it often appears after puberty.5 These patients often
present with azoospermia and have difficulty with fertility. However, the literature
provides little information about the fertility issues resulting from this syndrome.
Advances in assisted reproductive techniques have, in rare cases, allowed for the
production of offspring by patients with certain diagnoses thought to be associated
with universal infertility.6
7
Here, we report the case of a 30-year-old male patient with 48,XXYY syndrome who was
referred to our hospital in April 2016 for fertility treatment. In his family history,
he was the only child of healthy nonconsanguineous parent. His mother's pregnancy
and delivery were normal. The patient was born at term with normal measurements. We
noted that the patient had greater difficulties in understanding and developing social
relationships. He married three years before presentation but did not have children
at that time. However, there were no available data regarding his parent.
The patient had a height of 185 cm, a weight of 80 kg, a body mass index of 23.4 kg
m−2, and a blood pressure of 125/75 mmHg. The secondary sexual characteristics of
the patient are poorly developed, and he has some feminine characteristics, such as
no beard, less hair, and breast development. In addition, he presents orbital hypertelorism,
eunuchoid skeleton, reduced muscle mass, elongated arms and legs, and small testicles
and penis.
Laboratory investigations showed a normal blood cell count, normal thyroid-stimulating
hormone (TSH), iron and calcium levels, and abnormal hepatic, renal, and gonadal functions.
Most biological data from urine were within normal limits, with the exception of urinary
protein, urinary total protein/creatinine, urinary albumin/creatinine, microalbumin,
and 24 h urinary protein (urinary protein: 555.0 mg l−1; urinary total protein/creatinine:
286.5; urinary albumin/creatinine: 186.9; microalbumin: 362.5 mg l−1; and 24 h urinary
protein: 522 mg per 24 h). Thus, we diagnosed the patient with proteinuria resulting
from some unknown reason. Biological data revealed that cholesterol and triglycerides
were much higher than normal, suggesting the presence of hyperlipidemia (cholesterol:
6.87 mmol l−1; triglycerides: 5.74 mmol l−1). Hormonal data showed a low testosterone
level accompanied by elevated basal gonadotropin levels (
Table 1
), and these data were suggestive of a sex chromosome aneuploidy.
Table 1
Reproductive hormonal profile in the patient with 48,XXYY syndrome
We performed karyotype analysis twice for this patient using lymphocytes from peripheral
blood; 30 metaphases were counted in the first analysis (320–400 G-banding) and 100
metaphases were counted in the second analysis (550 G-banding). Results from the two
analyses showed the presence of the 48,XXYY aneuploidy in all the cells that were
analyzed (
Figure 1
). The result of Y chromosome microdeletion detection showed no deletion of the six
sequence tagged sites (sY84, sY86, sY127, sY134, sY254, sY255) and SRY gene, suggesting
that the AZF regions are complete. Although the patient suffers from azoospermia,
his family had a strong fertility requirement. Microdissection testicular sperm extraction
was successfully performed; surprisingly, normally shaped sperm were found under a
microscope after tearing of the seminiferous tubules.
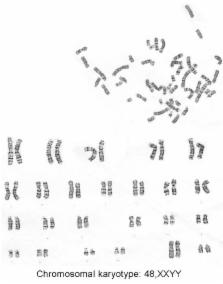
Figure 1
Chromosome test results.
Blood from the patient's wife was examined, and the results were consistent with the
experimental requirements. Under intravenous anesthesia, ovarian puncture ovulation
was carried out with the guidance of vaginal ultrasound imaging. Nine eggs were successfully
removed, six were mature, and four were fertilized by intracytoplasmic sperm injection.
Then two embryos developed into blastula stage and were frozen, followed by in vitro
fertilization with preimplantation genetic diagnosis. All the procedures were approved
by the Ethics Committee of our hospital, and the informed consent was obtained from
the patient and his spouse. The patient's spouse is currently successfully pregnant,
and the embryo is normal.
In this report, the patient had been married for three years and had conceived no
children even without contraception. Infertility was diagnosed, and the patient was
hospitalized at our center to address this issue. A microdissection for testicular
sperm extraction was performed for this patient with azoospermia. Ramasamy et al.8
demonstrated that increased male age is associated with a trend toward a lower sperm
retrieval rate in patients with Klinefelter's syndrome, and that various types of
preoperative hormonal therapies did not result in different sperm retrieval rates,
but men with a normal baseline testosterone level had the best sperm retrieval rate
of 86%. Fortunately, although the patient's hormone levels were abnormal and his testosterone
was low, normal sperm were nonetheless identified under the microscope after tearing
of the seminiferous tubules. The entire search process was difficult, but it was a
pleasant surprise that the screened sperm were nonprogressively motile and were normally
shaped. With in vitro fertilization, the sperm and egg successfully combined, and
embryonic development was progressing successfully at the time of the report.
Our case demonstrates the main typical features of 48,XXYY syndrome in a patient who
suffers from infertility. The patient has a strong fertility requirement. How to help
patients with 48,XXYY syndrome to have normal children has not been previously reported
in the literature. Fortunately, normal sperm were found in our patient under high-magnification
microscopy. Through the treatment of this case, it is proposed that microdissection
testicular sperm extraction is an effective sperm retrieval technique for men with
48,XXYY syndrome.
COMPETING INTERESTS
All authors declare no competing interests.
AUTHOR CONTRIBUTIONS
DFL, KH, and HJ conceived the study, performed the operation, and drafted the article.
KH, JMM, and LMZ performed the operation and participated in the acquisition of data.
YZY and ZZ contributed to clinical follow-up of the patient and helped the review
and editing of manuscript, and LMZ was responsible for the revision of the article.
All authors read and approved the final manuscript.
Related collections
Most cited references5
- Record: found
- Abstract: found
- Article: not found
Successful fertility treatment for Klinefelter's syndrome.
- Record: found
- Abstract: not found
- Article: not found
The 48,XXYY syndrome.
J. Nielsen, Kasper Sørensen, T Rølle … (1978)

- Record: found
- Abstract: found
- Article: found
48XXYY Syndrome in an Adult with Type 2 Diabetes Mellitus, Unilateral Renal Aplasia, and Pigmentary Retinitis
Baha Zantour, Mohamed Habib Sfar, Samia Younes … (2010)