- Record: found
- Abstract: found
- Article: found
Emerging viral infections in immunocompromised patients: A great challenge to better define the role of immune response
Read this article at
Abstract
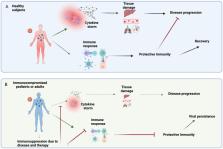
The immune response to invading pathogens is characterized by the rapid establishment of a complex network of cellular interactions and soluble signals. The correct balancing of activating and regulating pathways and tissue-homing signals determines its effectiveness and persistence over time. Emerging viral pathogens have always represented a great challenge to the immune system and an often uncontrolled/imbalanced immune response has been described (e.g. cytokine storm, immune paralysis), contributing to the severity of the disease. Several immune biomarkers and cell subsets have been identified as major players in the cascade of events leading to severe diseases, highlighting the rationale for host-directed intervention strategy. There are millions of immunocompromised pediatric and adult patients worldwide (e.g. transplant recipients, hematologic patients, subjects with primary immune-deficiencies), experiencing an impaired immune reactivity, due to diseases and/or to the medical treatments. The reduced immune reactivity could have two paradoxical non-exclusive effects: a weak protective immunity on one hand, and a reduced contribution to immune-mediated pathogenetic processes on the other hand. In these sensitive contexts, the impact of emerging infections represents a still open issue to be explored with several challenges for immunologists, virologists, physicians and epidemiologists. In this review, we will address emerging infections in immunocompromised hosts, to summarize the available data concerning the immune response profile, its influence on the clinical presentation, the possible contribution of persistent viral shedding in generating new viral variants with improved immune escape features, and the key role of vaccination.
Related collections
Most cited references80
- Record: found
- Abstract: found
- Article: not found
Dexamethasone in Hospitalized Patients with Covid-19 — Preliminary Report
- Record: found
- Abstract: found
- Article: found
COVID-19: consider cytokine storm syndromes and immunosuppression
- Record: found
- Abstract: found
- Article: not found