- Record: found
- Abstract: found
- Article: not found
Predictors of new-onset diabetic ketoacidosis in patients with moderate to severe COVID-19 receiving parenteral glucocorticoids: A prospective single-centre study among Indian type 2 diabetes patients
Read this article at
Abstract
Background and aim
COVID-19 infection predisposes to diabetic ketoacidosis(DKA); whether glucocorticoids enhances this risk is unknown. We aimed to study the occurrence of DKA after initiating glucocorticoids in patients with type 2 diabetes mellitus(T2DM) and moderate-to-severe COVID-19, and identify predictors for it.
Methods
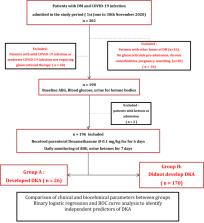
Patients with T2DM and moderate or severe COVID-19 infection were prospectively observed for development of new-onset DKA for one week following initiation of parenteral dexamethasone. Clinical and biochemical parameters were compared between those who developed DKA (Group A) and those who didnot (Group B). Logistic regression was done to identify independent risk-factors predicting DKA; ROC-curve analysis to determine cut-offs for the parameters in predicting DKA.
Results
Amongst 302 patients screened, n = 196 were finally included, of whom 13.2% (n = 26,Group A) developed DKA. Patients in Group A were younger, had lower BMI, increased severity of COVID-19 infection, higher HbA1c%, CRP, IL-6, D-dimer and procalcitonin at admission (p all < 0.02). Further, admission BMI (OR: 0.43, CI: 0.27–0.69), HbA1c % (OR: 1.68, CI: 1.16–2.43) and serum IL-6 (OR: 1.02, CI: 1.01–1.03) emerged as independent predictors for DKA. Out of these, IL-6 levels had the highest AUROC (0.93, CI: 0.89–0.98) with a cut-off of 50.95 pg/ml yielding a sensitivity of 88% and specificity of 85.2% in predicting DKA.
Related collections
Most cited references28
- Record: found
- Abstract: found
- Article: not found
Structure of the SARS-CoV-2 spike receptor-binding domain bound to the ACE2 receptor
- Record: found
- Abstract: found
- Article: not found
Are patients with hypertension and diabetes mellitus at increased risk for COVID-19 infection?
- Record: found
- Abstract: found
- Article: not found
