- Record: found
- Abstract: found
- Article: found
New WHO prevalence estimates of mental disorders in conflict settings: a systematic review and meta-analysis
Read this article at
Summary
Background
Existing WHO estimates of the prevalence of mental disorders in emergency settings are more than a decade old and do not reflect modern methods to gather existing data and derive estimates. We sought to update WHO estimates for the prevalence of mental disorders in conflict-affected settings and calculate the burden per 1000 population.
Methods
In this systematic review and meta-analysis, we updated a previous systematic review by searching MEDLINE (PubMed), PsycINFO, and Embase for studies published between Jan 1, 2000, and Aug 9, 2017, on the prevalence of depression, anxiety disorder, post-traumatic stress disorder, bipolar disorder, and schizophrenia. We also searched the grey literature, such as government reports, conference proceedings, and dissertations, to source additional data, and we searched datasets from existing literature reviews of the global prevalence of depression and anxiety and reference lists from the studies that were identified. We applied the Guidelines for Accurate and Transparent Health Estimates Reporting and used Bayesian meta-regression techniques that adjust for predictors of mental disorders to calculate new point prevalence estimates with 95% uncertainty intervals (UIs) in settings that had experienced conflict less than 10 years previously.
Findings
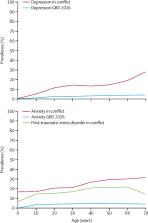
We estimated that the prevalence of mental disorders (depression, anxiety, post-traumatic stress disorder, bipolar disorder, and schizophrenia) was 22·1% (95% UI 18·8–25·7) at any point in time in the conflict-affected populations assessed. The mean comorbidity-adjusted, age-standardised point prevalence was 13·0% (95% UI 10·3–16·2) for mild forms of depression, anxiety, and post-traumatic stress disorder and 4·0% (95% UI 2·9–5·5) for moderate forms. The mean comorbidity-adjusted, age-standardised point prevalence for severe disorders (schizophrenia, bipolar disorder, severe depression, severe anxiety, and severe post-traumatic stress disorder) was 5·1% (95% UI 4·0–6·5). As only two studies provided epidemiological data for psychosis in conflict-affected populations, existing Global Burden of Disease Study estimates for schizophrenia and bipolar disorder were applied in these estimates for conflict-affected populations.
Related collections
Most cited references13
- Record: found
- Abstract: found
- Article: not found
60,000 disaster victims speak: Part I. An empirical review of the empirical literature, 1981-2001.
- Record: found
- Abstract: found
- Article: not found
Burden of depressive disorders by country, sex, age, and year: findings from the global burden of disease study 2010.

- Record: found
- Abstract: found
- Article: found