- Record: found
- Abstract: found
- Article: found
Management of Acute Submacular Hemorrhage with Intravitreal Injection of Tenecteplase, Anti-vascular Endothelial Growth Factor and Gas
Read this article at
Abstract
Purpose
To evaluate the visual and anatomical outcomes for neovascular age-related macular degeneration with submacular hemorrhage after intravitreal injections of tenecteplase (TNK), anti-vascular endothelial growth factor (VEGF) and expansile gas.
Methods
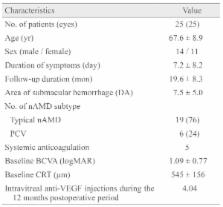
This study was a retrospective clinical case series following 25 eyes of 25 patients. All patients received a triple injection using 0.05 mL TNK (50 µg), 0.05 mL anti-VEGF and 0.3 mL of perfluoropropane gas. Retreatment with anti-VEGF was performed as needed. Preoperative and postoperative best-corrected visual acuity and central retinal thickness were analyzed.
Results
The mean logarithm of the minimum angle of resolution of best-corrected visual acuity improved significantly from 1.09 ± 0.77 at baseline to 0.52 ± 0.60 at 12 months ( p < 0.001). The mean central retinal thickness also improved significantly from 545 ± 156 at baseline to 266 ± 107 at 12 months ( p < 0.001). A visual improvement of 0.3 logarithm of the minimum angle of resolution unit or more was achieved in 15 eyes (60%). During the 12 postoperative months, an average of 4.04 intravitreal anti-VEGF injections was applied.
Related collections
Most cited references22
- Record: found
- Abstract: found
- Article: not found
Surgery for hemorrhagic choroidal neovascular lesions of age-related macular degeneration: ophthalmic findings: SST report no. 13.
- Record: found
- Abstract: found
- Article: not found
Factors prognostic of visual outcome in patients with subretinal hemorrhage.
- Record: found
- Abstract: found
- Article: not found