- Record: found
- Abstract: found
- Article: found
Harnessing immunotherapy for brain metastases: insights into tumor–brain microenvironment interactions and emerging treatment modalities
Read this article at
Abstract
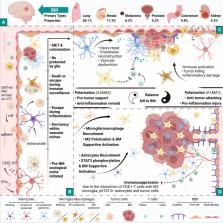
Brain metastases signify a deleterious milestone in the progression of several advanced cancers, predominantly originating from lung, breast and melanoma malignancies, with a median survival timeframe nearing six months. Existing therapeutic regimens yield suboptimal outcomes; however, burgeoning insights into the tumor microenvironment, particularly the immunosuppressive milieu engendered by tumor–brain interplay, posit immunotherapy as a promising avenue for ameliorating brain metastases. In this review, we meticulously delineate the research advancements concerning the microenvironment of brain metastases, striving to elucidate the panorama of their onset and evolution. We encapsulate three emergent immunotherapeutic strategies, namely immune checkpoint inhibition, chimeric antigen receptor (CAR) T cell transplantation and glial cell-targeted immunoenhancement. We underscore the imperative of aligning immunotherapy development with in-depth understanding of the tumor microenvironment and engendering innovative delivery platforms. Moreover, the integration with established or avant-garde physical methodologies and localized applications warrants consideration in the prevailing therapeutic schema.
Related collections
Most cited references225
- Record: found
- Abstract: found
- Article: not found
Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries
- Record: found
- Abstract: found
- Article: not found
Cancer statistics in China, 2015.
- Record: found
- Abstract: found
- Article: not found