- Record: found
- Abstract: found
- Article: found
Natural killer cell therapy for hematologic malignancies: successes, challenges, and the future

Read this article at
Abstract
The adoptive transfer of natural killer (NK) cells is an emerging therapy in the field of immuno-oncology. In the last 3 decades, NK cells have been utilized to harness the anti-tumor immune response in a wide range of malignancies, most notably with early evidence of efficacy in hematologic malignancies. NK cells are dysfunctional in patients with hematologic malignancies, and their number and function are further impaired by chemotherapy, radiation, and immunosuppressants used in initial therapy and hematopoietic stem cell transplantation. Restoring this innate immune deficit may lead to improved therapeutic outcomes. NK cell adoptive transfer has proven to be a safe in these settings, even in the setting of HLA mismatch, and a deeper understanding of NK cell biology and optimized expansion techniques have improved scalability and therapeutic efficacy. Here, we review the use of NK cell therapy in hematologic malignancies and discuss strategies to further improve the efficacy of NK cells against these diseases.
Related collections
Most cited references200
- Record: found
- Abstract: found
- Article: not found
Use of CAR-Transduced Natural Killer Cells in CD19-Positive Lymphoid Tumors
- Record: found
- Abstract: found
- Article: found
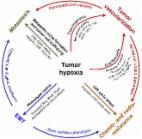
The role of hypoxia in cancer progression, angiogenesis, metastasis, and resistance to therapy
- Record: found
- Abstract: not found
- Article: not found