- Record: found
- Abstract: found
- Article: found
Unusual localization of bleeding under acenocoumarol: Spinal subdural hematoma
Read this article at
Highlights
-
•
The spinal subdural hematoma is a rare situation which should be evoked in any patient treated by vitamin K antagonists with signs of spinal cord compression.
-
•
Magnetic resonance imaging is the imaging exam of choice to establish the diagnosis.
-
•
Rapid correction of bleeding disorders is required.
-
•
Sometimes, emergent surgical evacuation of the hematoma is the only therapeutic option to ensure optimal neurological prognosis.
-
•
The procedures for resuming anticoagulation should be subject to a multidisciplinary consultation.
Abstract
Background
The spinal subdural hematoma (SSH) is an extremely rare entity which represents only 4.1% of all spinal hematomas. It needs accurate diagnosis and rapid intervention because of the major neurological risk induced by spinal compression. Several etiologies have been reported: anticoagulant treatments, haematological disorders, arterio-venous malformation, repeated attempts at lumbar punctures and tumors. We report the case of an 82-year-old patient under acenocoumarol for atrial fibrillation who presented with paraplegia secondary to SSH.
Case report
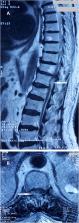
An 82-year-old patient with a history of ischemic heart disease and atrial fibrillation under acenocoumarol was admitted to emergency department with sudden onset of paraplegia and intense back pain associated with urinary incontinence and anal sphincter disorder. On examination his lower limb power was MRC grade 0 out of 5 in all ranges of movement bilaterally and a complete bilateral anesthesia reaching the T12 dermatome was noted. Biological test results showed an International Normalized Ratio at 10. Magnetic resonance imaging revealed a posteriorly located spinal hematoma at T12 level, measuring 36 mm with spinal cord compression. After correction of hemostasis disorders the patient was admitted to the operating room for a T11-L1 laminectomy with evacuation of the subdural hematoma. Muscle power showed a gradual improvement in the lower limbs estimated at 3/5 with regression of sphincter disorders but unfortunately a sequellar sensory impairment persisted.
Related collections
Most cited references20
- Record: found
- Abstract: found
- Article: not found
Spinal hematoma: a literature survey with meta-analysis of 613 patients.
- Record: found
- Abstract: found
- Article: not found
The pharmacology and management of the vitamin K antagonists: the Seventh ACCP Conference on Antithrombotic and Thrombolytic Therapy.
- Record: found
- Abstract: found
- Article: not found