- Record: found
- Abstract: found
- Article: found
Chronic traumatic encephalopathy in a former Australian rules football player diagnosed with Alzheimer’s disease
letter
Alan J. Pearce
1 ,
Joanne Sy
2 ,
Maggie Lee
2
,
3 ,
Antony Harding
2
,
3 ,
Rowena Mobbs
3
,
4 ,
Jennifer Batchelor
4 ,
Catherine M. Suter
2 ,
Michael E. Buckland
2
,
3
,
26 February 2020
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
To the Editor:
The first case report of chronic traumatic encephalopathy (CTE) in a National Football
League player in 2005 [9] opened the floodgates for the identification of CTE in American
football. CTE is now reported in ex-players of other contact sports, including ice
hockey, soccer, rugby union, and most recently in Australian rugby league [2]. To
date, repetitive head injury remains the only known risk factor for the development
of CTE [3]. Here we describe the first case of CTE in Australian rules football (ARF),
the most popular contact sport in Australia.
The decedent was a male in his 9th decade who had played more than 350 first-grade
matches of ARF over 19 years. At age 64 he was diagnosed with Alzheimer’s disease
(AD), with accompanying personality change, depression and anger/aggression issues
around this time. He had been diagnosed with REM sleep behaviour disorder several
years prior to his presumptive AD diagnosis. His cognitive issues were dominated by
memory loss, which was slowly progressive until a distinct acceleration in the last
~ 5 years of life. Mild Parkinsonian features of uncertain aetiology were identified
several years after his AD diagnosis, possibly related to low-dose antipsychotic medication.
He also had intercurrent ischaemic heart disease, hypercholesterolaemia, and hypertension,
all of which were well managed. He did not use alcohol, tobacco, or illicit drugs.
Table 1 summarises the relevant neuropathology. There was mild-moderate frontal and
temporal lobe atrophy with ex-vacuo ventriculomegaly (lateral and third ventricles),
mild uncomplicated atheroma in the basal vasculature, and pallor of the substantia
nigra. Phosphorylated Tau immunoreactivity (pTau) was present in many grey matter
regions. Neocortical pTau was markedly concentrated in an irregular perivascular distribution
at sulcal depths in the soma and processes of both neurons and astrocytes: this is
the defining lesion of CTE [8] (Fig. 1a, b). Twelve CTE foci were present within nine
frontal lobe blocks, and four foci in four temporal lobe blocks. In the temporal and
insular cortices there was also dense involvement of superficial layers (layers II-III)
(Fig. 1c), consisting of pretangle and tangle pTau, and some ghost tangles. This pattern
of pTau deposition, commonly seen in severe CTE, is distinct from the typical pTau
deposition in AD (Fig. 1d). Neuronal pTau was composed of both 3R and 4R isoforms,
while astrocytic pTau was predominantly 4R.
Table 1
Summary of neuropathology findings
Tau pathology
Depths of cortical sulci, perivascular
neuronal, astrocytic, neuritic
frontal +++
temporal ++
parietal, occipital -
Prominent superficial neocortical layers
neuronal, astrocytic, neuritic
temporal +++
insular +++
frontal +
parietal, occipital -
Hippocampus
neuronal
CA2, CA4 +++
CA3 ++
DG +
CA1 sclerosis (astrocytic) +
Amygdala neuronal, neuritic
+++
Striatum, Lentiform nuclei neuronal, neuritic
+
Thalamus neuronal, neuritic
+
Hypothalamus incl. Mammillary body
neuronal, neuritic
+++
Midbrain neuronal, neuritic
substantia nigra +++
median raphe +++
tectum ++
Pons
locus coeruleus +
abducens nucleus +
Medulla
–
Cerebellum
–
Subpial & periventricular ARTAG
present
Ghost tangles
CA1, entorhinal, superficial temporal, amygdala
pTDP-43 pathology
NCI, neuritic
amygdala ++
hippocampus +
superficial temporal ++
depths of frontal sulci +
Other pathology
Vascular disease, arteriolosclerosis
Vascular disease, atherosclerosis
basal ganglia +++
subcortical white matter +++
basal vessels +
Beta-A4 (amyloid)
Thaal 4 (A3)
CERAD score
C2
Alpha-synuclein
absent
Diagnosis
CTE Stage III
AD-NC (A3, B2, C2)
CA cornu ammonis, DG dentate gyrus, NCI neuronal cytoplasmic inclusions, AD-NC Alzheimer’s
Disease neuropathologic change, ARTAG aging-related tau astrogliopathy
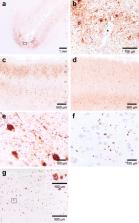
Fig. 1
Immunohistochemical findings. a, b pTau (clone AT8, 1:800 dilution) immunoreactivity
concentrated at the depths of a cortical sulcus in the superior frontal cortex (Brodmann
area 8). pTau is found in the soma and processes of both neurons and astrocytes in
an irregular distribution concentrated around blood vessels: the defining lesion of
CTE. The boxed area in (a) is represented at high power in (b). c pTau staining of
anterior superior temporal lobe (Brodmann area 38), showing dense immunoreactivity
of both neurons and astrocytes concentrated in superficial cortical layers (layers
II-III). This superficial pTau is more evenly distributed throughout temporal cortex,
with only occasional denser foci at sulcal depths (four foci across four blocks of
anterior temporal lobe). pTau is also present in deeper cortical layers as irregular/patchy
clumps of mixed neuronal and astrocytic staining. d Inferior temporal gyrus from another
individual (77yo ex-ARF player with AD but no CTE), showing a pattern of pTau pathology
distinct to that of CTE, with neuronal pTau staining concentrated in deeper cortical
layers and dense neuritic staining.
e Widespread pTau staining (as both globose tangles and pretangle pathology) in neurons
of the substantia nigra, with accompanying neuritic pathology. There was accompanying
moderate neuronal loss, pigment incontinence and gliosis. f pTDP-43 (clone 1D3, 1:500
dilution) staining of temporal lobe in the same superficial cortical layers depicted
in (c), showing positive neuronal cytoplasmic inclusions and short neurites. g Beta-amyloid
(betaA4 clone 6F/3D, 1:50 dilution) immunoreactivity in superior frontal cortex (Brodmann
area 8). The boxed area is represented at high power in the inset. All immunohistochemistry
performed on 4 μm sections from standard-sized blocks of formalin-fixed (10% neutral
buffered formalin), paraffin-embedded tissue on a Leica BOND-MAX™ autostainer using
the Leica BOND Polymer Refine detection system as per the manufacturer’s recommendations
Hippocampal sclerosis was present, with some ghost tangles, gliosis, and heavy pTau
involvement. Widespread neuronal and neuritic pTau was also present in amygdala, medial
hypothalamic nuclei, mammillary body, nucleus basalis, substantia nigra (Fig. 1e),
raphe nuclei and colliculi. Subpial and subependymal pTau in thorn-shaped astrocytes
was present, consistent with aging-related tau astrogliopathy (ARTAG), most prominent
in the temporal lobe.
Phosphorylated TDP-43 was present as neuronal cytoplasmic inclusions and short neurites,
and was colocalised with regions of severe CTE pathology (Fig. 1f), a common finding
in CTE [8]. Beta-amyloid and neuritic plaques were seen, corresponding to Thaal phase
4 (A3; Fig. 1g), and CERAD score of C2. While pTau pathology was in the typical distribution
of CTE rather than AD, assessing all neurofibrillary tangle pathology gave a Braak
stage of IV (B2). Together this equated to intermediate AD-neuropathologic change
(A3,B2,C2) [6]. Immunohistochemistry for alpha-synuclein was negative.
Severe arteriolosclerosis was present in basal ganglia and white matter. Rarefaction
and gliosis in subcortical white matter was generally mild-moderate, while in the
anterior commissure and external capsule it was severe. Axonal pTau was moderate in
these above two tracts, and mild elsewhere, and was seen as immunoreactive neurites
and axonal varicosities. Beta-amyloid precursor protein was absent from anterior commissure
and external capsule, and present in internal capsule in a pattern consistent with
agonal changes only.
Taken together, these findings demonstrate severe (Stage III) CTE. This is the first
confirmed case in ARF. CTE was associated with early-onset dementia, with neuropsychological
features commonly described in pathologically confirmed CTE cases from other sports.
Typical CTE pathology in this case was accompanied by intermediate AD-neuropathologic
change, and severe small vessel disease.
ARF is the most popular contact sport in Australia, with a player base of more than
1.5 million, and a significant (30%) female representation. ARF is characterized by
its fast-paced physicality: it involves running at speed, frequent jumping, and high-impact
landing. With 18 players per side high-force collisions are commonplace, and can occur
in any direction, on the ground or in the air. Thus unsurprisingly, ARF has a high
injury and concussion rate [7], and the unique nature of the game places players at
risk of head injury from multiple and complex mechanisms, distinct from those of the
rugby codes. The limited available evidence on long-term neurological outcomes of
ARF players suggests that, like ex-athletes of other contact sports, they too are
predisposed to develop persisting deficits in motor control and cognition [4, 10].
There are no criteria for distinguishing AD-associated from CTE-associated pTau pathology
when there is intercurrent disease. The identification of conformational differences
in the β-helix region of pTau in CTE versus AD [5] suggests that these are two distinct
pathologies, but currently all neurofibrillary tangle pathology in a CTE case is assessed
to derive a Braak stage for AD. This ‘double-counting’ of pTau is likely to overestimate
the severity of co-occurring AD in CTE, particularly in older individuals such as
described here. Development of conformation-specific antibodies specific for CTE-pTau
would greatly assist in distinguishing these two diseases.
This case represents only the second ARF player brain donated to the recently established
Australian Sports Brain Bank [1], and the first to be diagnosed with CTE. While we
can make no claims of CTE incidence in ARF based on this index case, the distinctive
and severe pTau pathology is something we have not encountered in our busy clinical
practice outside of ex-contact sports players [2]. That it exists at all should serve
as a call to action to recognise and research CTE, and the very clear association
with repetitive head injury. Claims of a lack of demonstrated ‘causality’ are unhelpful,
and arguably irrelevant when assessing a public and occupational health issue such
as CTE.
Related collections
Most cited references5
- Record: found
- Abstract: found
- Article: not found
Chronic traumatic encephalopathy in a National Football League player.
Bennet Omalu, Steven Dekosky, Ryan L Minster … (2005)

- Record: found
- Abstract: found
- Article: found
White matter capillaries in vascular and neurodegenerative dementias
Yoshiki Hase, Ren Ding, Gina Harrison … (2019)
- Record: found
- Abstract: found
- Article: not found
The long-term effects of sports concussion on retired Australian football players: a study using transcranial magnetic stimulation.
Alan Pearce, Kate E. Hoy, Mark Rogers … (2014)