- Record: found
- Abstract: found
- Article: found
Effect of Preoperative Opioid Use on Adverse Outcomes, Medical Spending, and Persistent Opioid Use Following Elective Total Joint Arthroplasty in the United States: A Large Retrospective Cohort Study of Administrative Claims Data
Read this article at
Abstract
Objective
Between 17% and 40% of patients undergoing elective arthroplasty are preoperative opioid users. This US study analyzed patients in this population to illustrate the relationship between preoperative opioid use and adverse surgical outcomes.
Subjects
Adults (aged 18+) who received elective total knee, hip, or shoulder replacement in 2014–2015.
Methods
A patient was a preoperative opioid user if opioid prescription fills occurred in two periods: 1–30 and 31–90 days presurgery. Zero-truncated Poisson (incidence rate ratio [IRR]), logistic (odds ratio [OR]), Cox (hazard ratio [HR]), and quantile regressions modeled the effects of preoperative opioid use and opioid dose, adjusted for demographics, comorbidities, and utilization.
Results
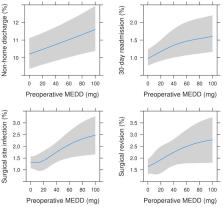
Among 34,792 patients (38% hip, 58% knee, 4% shoulder), 6,043 (17.4%) were preoperative opioid users with a median morphine equivalent daily dose of 32 mg. Preoperative opioid users had increased length of stay (IRR = 1.03, 95% CI = 1.02 to 1.05), nonhome discharge (OR = 1.10, 95% CI = 1.00 to 1.21), and 30-day unplanned readmission (OR = 1.43, 95% CI = 1.17 to 1.74); experienced 35% higher surgical site infection (HR = 1.35, 95% CI = 1.14 to 1.59) and 44% higher surgical revision (HR = 1.44, 95% CI = 1.21 to 1.71); had a median $1,084 (95% CI = $833 to $1334) increase in medical spend during the 365 days after discharge; and had a 64% lower rate of opioid cessation (HR = 0.34, 95% CI = 0.33 to 0.35) compared with patients not filling two or more prescriptions across periods.
Conclusions
Preoperative opioid users had longer length of stay, increased revision rates, higher spend, and persistent opioid use, which worsened with dose. Adverse outcomes after elective joint replacement may be reduced if preoperative opioid risk is managed through increased monitoring or opioid cessation.
Related collections
Most cited references26
- Record: found
- Abstract: found
- Article: not found
Trends in Opioid Analgesic-Prescribing Rates by Specialty, U.S., 2007-2012.
- Record: found
- Abstract: not found
- Article: not found
Pharmaceutical overdose deaths, United States, 2010.
- Record: found
- Abstract: not found
- Article: not found