- Record: found
- Abstract: found
- Article: found
Outbreak of Salmonella Heidelberg Infections Linked to a Single Poultry Producer — 13 States, 2012–2013
research-article
Margaret Grinnell ,
Ginger Provo
Nicola Marsden-Haug , MPH,
Kathleen A. Stigi , MPH
Emilio DeBess , DVM
Bonnie Kissler , MPH
Emily Crarey , MPH,
Heather Tate , PhD
Jeshua Pringle , MPH,
Julian Grass , MPH,
Jason Folster , PhD,
Ian Williams , PhD,
Laura Gieraltowski , PhD
Alison S. Laufer , PhD
12 July 2013
Read this article at
There is no author summary for this article yet. Authors can add summaries to their articles on ScienceOpen to make them more accessible to a non-specialist audience.
Abstract
In June 2012, the Oregon Health Authority and the Washington State Department of Health
noted an increase in the number of Salmonella enterica serotype Heidelberg clinical
isolates sharing an identical pulsed-field gel electrophoresis (PFGE) pattern. In
2004, this pattern had been linked to chicken from Foster Farms by the Washington
State Department of Health; preliminary 2012 interviews with infected persons also
indicated exposure to Foster Farms chicken. On August 2, 2012, CDC’s PulseNet* detected
a cluster of 19 Salmonella Heidelberg clinical isolates matching the outbreak pattern.
This report summarizes the investigation by CDC, state and local health departments,
the U.S. Department of Agriculture’s Food Safety and Inspection Service (USDA-FSIS),
and the Food and Drug Administration (FDA) and reinforces the importance of safe food
handling to prevent illness. A total of 134 cases from 13 states were identified,
including 33 patients who were hospitalized. This multifaceted investigation used
standard epidemiologic and laboratory data along with patient shopper card purchase
information, and PFGE data from the retail meat component of the National Antimicrobial
Resistance Monitoring System (NARMS)†, a relatively novel tool in outbreak investigation,
to link the outbreak strain to chicken from Foster Farms.
Epidemiologic Investigation
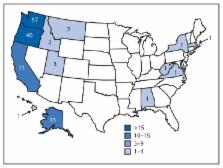
A total of 134 persons infected with the Salmonella Heidelberg outbreak strain§ with
illness onset on or after June 1, 2012, were identified in 13 states (Figure 1). Median
patient age was 22 years (range: <1 to 94 years); 73 (55%) of 132 patients with data
available were female. Illness onset ranged from June 4, 2012, to April 16, 2013.
Thirty-three (31%) of 105 patients with known outcomes were hospitalized; no deaths
were reported. The majority of cases were reported from four states in the Pacific
Northwest: Washington, 57 cases; Oregon, 40; Alaska, 13; and California, 11 (Figure
1). This outbreak appears to have ended, based on the calculated 5-year baseline of
the expected number of cases reported per week.
Initial state-based interviews found that chicken was commonly consumed by the persons
with infections. A structured questionnaire was developed to collect detailed information
on chicken and other exposures noted during initial interviews, and exposures commonly
linked to Salmonella Heidelberg, such as eggs. Of 70 patients who responded, 55 (79%)
reported consuming chicken in the week before illness onset, a percentage significantly
higher (p=0.01) than the 64.9% reported in the 2006–2007 Foodborne Diseases Active
Surveillance Network (FoodNet) Population Survey of healthy persons.¶ In addition,
eight patients reported that chicken had been prepared in the home, but either had
not been consumed or consumption was not specified. In total, 36 (71%) of 51 patients
who had brand information available reported exposure either to Foster Farms chicken
(27 patients) or to another brand likely produced by Foster Farms (although packaging
information was unavailable) (nine patients). Other exposures of interest (e.g., eggs)
were reported in significantly lower proportions by patients than by respondents to
the FoodNet survey.
NARMS, a collaboration of CDC, FDA’s Center for Veterinary Medicine, USDA, and participating
state public health laboratories, monitors the prevalence and trends of antimicrobial
resistance among enteric bacteria from humans, raw unprocessed retail meats, and food
animals. Of 14 clinical isolates from this outbreak tested for antimicrobial susceptibility
by NARMS, 12 were susceptible to all antimicrobials tested, and two were resistant
to amoxicillin/clavulanic acid, ampicillin, cefoxitin, ceftiofur, and ceftriaxone.
The two patients with resistant isolates both were aged <12 months and required hospitalization;
for both patients, exposure to Foster Farms chicken was reported. Resistance was mediated
by the presence of an IncI1 plasmid carrying a bla
CMY-2 gene. Plasmids are mobile genetic elements that can be gained or lost relatively
easily, which might explain the variable resistance profiles. Resistance to third-generation
cephalosporins (e.g., ceftriaxone) is clinically important because extended-spectrum
cephalosporins are commonly used for treatment of severe salmonellosis in children
(1).
Product Testing and Traceback Investigation
Oregon and Washington worked with USDA-FSIS to conduct a traceback investigation using
shopper card records from nine patients. Records indicated all nine patients purchased
Foster Farms chicken before illness onset. Four intact (i.e., unopened) chicken samples
from three Washington patients’ homes were tested for Salmonella; all yielded the
outbreak strain and were traced back to two Foster Farms slaughter establishments.
Three were susceptible to all antimicrobials tested; one was resistant to gentamicin,
streptomycin, and sulfisoxazole. As part of this investigation, USDA-FSIS sent an
incident investigation team to one Foster Farms slaughter establishment; the results
of that investigation have not yet been finalized.
NARMS Retail Samples
The NARMS retail meat surveillance program isolated the outbreak strain from Foster
Farms retail chicken samples purchased in Washington and Oregon in October 2012. Using
PFGE data provided by the Center for Veterinary Medicine, the association between
Foster Farms chicken and the outbreak strain was evaluated. From 2002 to 2011, Salmonella
was isolated from 1,503 (13%) of 11,417 retail chicken samples tested by NARMS, of
which 233 (16%) were serotype Heidelberg. Among these, 48 (21%) matched the outbreak
strain, of which 47 (98%) were Foster Farms retail chicken isolates. Stratification
by brand showed that 47 (52%) of 90 NARMS Foster Farms chicken isolates matched the
outbreak strain, compared with one (0.7%) of 143 isolates not from Foster Farms (p<0.001).
Public Health Response
The two state health departments and CDC issued Internet announcements and news releases
regarding the outbreak investigation, indicating that Foster Farms chicken was the
most likely source of the outbreak, that antimicrobial testing revealed most of the
isolates were susceptible to all antimicrobial agents tested, and reminding the public
of the importance of safe handling of raw poultry.
What is already known on this topic?
Poultry is the commodity most frequently associated with Salmonella outbreaks. Salmonella
is the most common bacterial cause of foodborne illness in the United States, and
is estimated to cause approximately 1 million illnesses annually.
What is added by this report?
An outbreak of 134 Salmonella Heidelberg cases in the Pacific Northwest was linked
to chicken consumption. Information from National Antimicrobial Resistance Monitoring
System (NARMS) retail meat surveillance and shopper card records helped link the outbreak
strain with Foster Farms.
What are the implications for public health practice?
The historical significance of this pattern in the Pacific Northwest suggests the
need for ongoing surveillance and intervention to prevent additional illnesses. Shopper
card records and NARMS retail meats surveillance can provide brand information crucial
to investigations of outbreaks linked to commonly consumed foods. Because it is not
unusual that raw poultry from any producer has Salmonella, it is important to continue
to remind consumers of the need for safe raw poultry handling practices to help the
public protect themselves and others from foodborne illness.
Editorial Note
Epidemiologic data, traceback investigations, and product testing support the conclusion
that Foster Farms chicken was the likely source of this outbreak. Shopper card records
collected from patients provided specific brand information for chicken, a commonly
consumed food product, and were critical to linking this outbreak to a single chicken
producer. The NARMS retail meat surveillance program not only isolated the outbreak
strain from Foster Farms retail chicken samples purchased in Oregon and Washington
during the current outbreak, but also demonstrated that 98% of historic isolates matching
the outbreak strain were from Foster Farms retail chicken samples. One limitation
to these findings is that they might not reflect all establishments that produce Foster
Farms chicken or all brands of chicken produced by each establishment.
PulseNet data collected before this outbreak indicate that four to eight human isolates
of this Heidelberg pattern typically are uploaded each month from June to November
(Figure 2). During this outbreak, an average of 12 human isolates matching the outbreak
strain was uploaded each month. The proportion of Salmonella Heidelberg human isolates
uploaded to PulseNet with this PFGE pattern also has been increasing: from 3.5% to
5.7% of all Salmonella Heidelberg uploads per year during 2004–2008, to 3.7% to 13.7%
during 2009–2012.
Historically, reports of this pattern to PulseNet come from the Pacific Northwest
region of the United States. Foster Farms chicken was previously linked to illness
in a 2004 investigation by Washington and USDA-FSIS (Kathryn MacDonald, Washington
State Department of Health, personal communication, 2012). USDA-FSIS conducted comprehensive
food safety assessments in 2004 and 2009. Following the 2004 assessment, USDA-FSIS
issued a Notice of Intended Enforcement to Foster Farms, after which uploads to PulseNet
of the outbreak strain decreased, followed by an increase in 2009 (Figure 3). From
2001 to 2012, Salmonella was isolated from 3,094 (4%) of 83,743 raw meat and poultry
samples collected for testing by USDA-FSIS from establishments in the western United
States. Among these, 264 (9%) were serotype Heidelberg, 45 (17%) of which matched
the outbreak strain. The historical significance of this pattern in the Pacific Northwest
suggests the need for ongoing surveillance and intervention to prevent additional
illnesses.
Salmonella Heidelberg is frequently isolated from retail meats and predominantly from
poultry products; in 2010, 38% of Salmonella Heidelberg strains isolated from retail
chicken breasts were resistant to at least one antimicrobial class (2). Raw poultry
in general can have Salmonella, and Salmonella is not considered a bacterial contaminant
in raw poultry from a regulatory perspective. However, poultry is the commodity most
often associated with Salmonella outbreaks (3). Therefore, consumers should follow
safe handling instructions to help protect themselves and others from foodborne illness.
USDA-FSIS set stricter pathogen-reduction performance standards for Salmonella contamination
in young chicken and turkey carcasses at slaughter facilities, effective July 2011.
In December 2012, USDA-FSIS announced that all establishments producing not-ready-to-eat
ground or comminuted poultry products, including Foster Farms, will be required to
reassess their Hazard Analysis and Critical Control Points plans, in response to recent
turkey-associated outbreaks of salmonellosis (4,5).
This outbreak illustrates the importance of a multifaceted outbreak investigation,
and particularly the value of incorporating historical PulseNet and NARMS data with
information from patient interviews, shopper card records, and product samples from
patients’ homes. NARMS retail meat surveillance data is a relatively novel and useful
tool to help link an outbreak strain with a particular brand and should be considered
in future foodborne disease outbreak investigations.
Related collections
Most cited references5
- Record: found
- Abstract: found
- Article: not found
Surveillance for foodborne disease outbreaks--United States, 2008.
- Record: found
- Abstract: not found
- Article: not found
New Performance Standards for Salmonella and Campylobacter in Young Chicken and Turkey Slaughter Establishments: Response to Comments and Announcement of Implementation Schedule
(2011)